 In January 2013, University Hospitals Rainbow Babies & Children’s Hospital launched the Rainbow Care Connection, a pediatric accountable care organization (ACO) with a $12.7 million CMS innovation grant to support children in Northeast Ohio, a third are enrolled in Medicaid. This innovative ACO has developed several successful mobile health initiatives to drive care collaboration with patients as part of their Physician Extension Team. This blog focuses on two key mobile health initiatives; iPads Minis for children with complex chronic conditions and HealthSpotSM, a community- based telemedicine kiosk.
In January 2013, University Hospitals Rainbow Babies & Children’s Hospital launched the Rainbow Care Connection, a pediatric accountable care organization (ACO) with a $12.7 million CMS innovation grant to support children in Northeast Ohio, a third are enrolled in Medicaid. This innovative ACO has developed several successful mobile health initiatives to drive care collaboration with patients as part of their Physician Extension Team. This blog focuses on two key mobile health initiatives; iPads Minis for children with complex chronic conditions and HealthSpotSM, a community- based telemedicine kiosk.
iPad Mini For Care Collaboration
“We wanted to help children with chronic medical conditions, especially those who have difficulty speaking or getting around. For children that cannot walk, it is challenging to get them to the office. By giving them an iPad Mini, these children are able to communicate with their care team including physicians, nurses, social workers and dieticians”, explains Dr. Richard Grossberg, Medical Director of University Hospitals Center for Comprehensive Care. “Our goal with this project is to reduce office and ER visits with this video connectivity.”
 In partnership with UH’s Rainbow Care Connection, the Center for Comprehensive Care strives to pioneer innovative ways to support children with complex chronic conditions, which can often seem overwhelming from a family’s perspective. As medical care continues to grow more complex, healthcare professionals acknowledge that families may need support beyond the clinic and hospital walls in order to be successful.
In partnership with UH’s Rainbow Care Connection, the Center for Comprehensive Care strives to pioneer innovative ways to support children with complex chronic conditions, which can often seem overwhelming from a family’s perspective. As medical care continues to grow more complex, healthcare professionals acknowledge that families may need support beyond the clinic and hospital walls in order to be successful.
Children with complex chronic conditions make up about 5% of children who access health care services but account for up to 50% of Medicaid dollars spent. “We were looking for an additional layer to outpatient care; providing families with an opportunity to manage less acute issues in the comfort of their own home”, Dr. Grossberg shares. “Launched in December 2013, we felt that video calls would be the most innovative and cost effective solution to accomplish this and have currently distributed 10 iPad mini devices to families.”
How do video calls work? A family uses their iPad mini to conduct a “video call” with the office. During their telemedicine visit, a Comprehensive Care nurse helps the family triage what is happening and can resolve or escalate care to a physician/nurse practitioner or acute care setting when needed. Additional applications of the video call are being trialed including conducting nutritional counseling and education by UH’s Comprehensive Care dietitians and therapeutic counseling completed by their Comprehensive Care social workers.
After the video call, the visit summary is documented and sent to the patient’s PCP. If a video call is escalated to include an ED or hospitalization, the UH acute care team has full electronic access to all of the video calls and assessment notes. Having the necessary tools to help guide a family though those moments when their child’s complex conditions go awry and help them overcome barriers to care is critical to helping families receive better care, achieve better health and gain a healthcare partner to share in their patient experiences.
HealthSpotSM Station
UH’s Rainbow Care Connection aims to reduce ER costs by finding new ways to support patients who go the ER with minor medical problems.

“Since we know that 70% of Medicaid patients in the ER can be managed in a less acute setting, we were looking for an alternative to provide access to care after hours. We wanted to test offering a solution in a community setting to see if this population would feel more comfortable getting after hours care in their own neighborhood rather than from a medical setting. We felt that telemedicine would be the most cost effective solution to accomplish this”, shares Dr. Andrew Hertz, Medical Director of University Hospitals Rainbow Care Connection. We had already piloted a HealthSpotSM kiosk running in our clinic and were ready to place a kiosk into a community setting”, Dr. Hertz explains.
“We decided on the HealthSpotSM kiosk vs other telemedicine units because of the incredible patient experience provided by the HealthSpotSM unit, including diagnostic equipment and the ability to transmit real-time vital signs and physical images.” Dr. Hertz and his team thought carefully about where to place the kiosk. “We started with a zip code analysis of patients coming into our ER to select potential locations and met with Community Neighborhood Association Leaders to discuss options. We chose the Friendly Inn Settlement (community building) in Cleveland and launched the program in October 2013.”
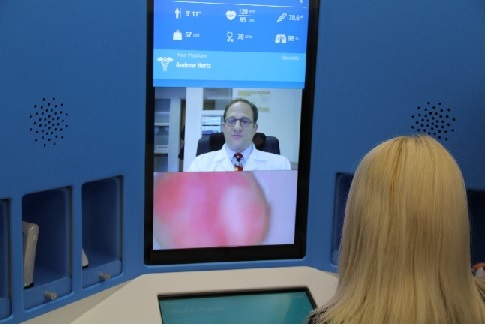
How does the HealthSpotSM kiosk work? A patient and their family members step into the fully enclosed kiosk with a medical assistant who helps support them during their high-definition video conference visit with the doctor who may be located a few towns away. “Our doctor is on the computer screen, with video and audio connectivity to instruments (i.e. scale, blood pressure cuff, stethoscope, otoscope, thermometer, dermascope, pulse oximeter) and decides which tools to use and when by unlocking the door at the right time. It is cool when they unlock it. It is magical to see the door open and the instrument there. Our patients and their families see what physician is seeing as they use their different devices. It is a wonderful educational experience”, describes Dr. Hertz.
Patients use the HealthSpotSM kiosk to take care of minor ailments and get check-ups, as an alternative to an emergency room visit. A parent/guardian can accompany a child from age three to 18 during their visit to the UH Rainbow HealthSpotSM station during weekdays from 5:30 – 11 p.m. and weekends from 1 – 11 p.m.
Since the launch of HealthSpotSM, Dr. Hertz and his team at UH have met with over 50 patients, with problems including rashes, fever, strep throat and pink eye.
After the remote appointment with the doctor, the visit summary is documented and sent manually to the patient’s PCP. “Our physicians currently document the visit on paper and fax it to the PCP who may be outside of the UH network. Over 50% of these patients are not in UH Rainbow’s system so we share their information like a retail clinic. We have an interest in having HealthSpotSM integrate this visit information into our hospital EMR,” explains Dr. Hertz.
“Anytime we can spend time with a patient in their own environment, we can better understand and address their needs.” Dr. Hertz adds that by understanding why patients choose the ER as their source of care enables his team to identify opportunities to change that behavior and meet patient needs. Certainly, having after-hours access to quality care in the inner city is valued by patients since the ER is often their only after-hours option.
Patients and family caregivers have had a very positive experience with the telemedicine visit within UH’s HealthSpotSM kiosk. 85% have indicated that if they did not have the HealthSpotSM visit, they would have gone to the ER. Over 90% would use it again. Here are some comments around value of the visit to them:
It's convenient and less time consuming.
I love the equipment and technology.
The one on one with the doctor.
That you get to see what's going on inside the little areas most doctors won't show you.
Close to home and speed of service.
Very helpful for my community.
Future Opportunities for UH Patient & Family Engagement
The team at the UH Rainbow Babies & Children’s Hospital Rainbow Care Connection is already planning ways to use the HealthSpotSM kiosk to bring care access to other patient populations. “Next we want to use telemedicine to enhance access to care in rural areas, where there are not a lot of specialists or after hours care options. We are planning to place a kiosk in a community building or a school”, Dr. Hertz adds.
In addition to expanding the HealthSpotSM kiosks, Dr. Hertz is interested in finding patient engagement tools that will help patients receive care through their phones to support the lower social economic population that tends to own mobile phones rather than computers. “No one has developed the mobile app for patients to receive care through smart phones which would enable a ‘meaningful clinical interaction’,” concludes Dr. Hertz.