You cannot turn on the television or look at a newspaper today without being reminded of the obesity epidemic facing our nation. According to a CDC study, over 37% of U.S. adults are obese, while about 70% are overweight.
Obesity has been associated with certain chronic conditions such as diabetes (type 2), cardiovascular disease and stroke. Last summer, American Medical Association classified Obesity as a disease, and the National Heart, Lung and Blood Institute recently published guidelines recommending that primary care physicians provide obesity counseling to all patients with Body Mass Index over 25 (which classifies them as overweight).
Many Americans try to lose weight but do not have the tools or professional guidance to be successful. Most physicians don’t have the training or tools to provide a comprehensive weight management program in their practice, and sometimes refer patients to commercial programs that are not clinically supervised.
RediClinic has stepped in to help. “We have developed a medically supervised program which is not just about weight loss but about health management”, explains Danielle Barrera, Chief Operating Officer at RediClinic. “When we developed this program in 2009, we noticed that many programs on the market were missing critical elements of a successful weight management program, and did not incorporate healthcare professionals, who are well positioned to have a significant impact on their patients’ lifestyle and health decisions.”
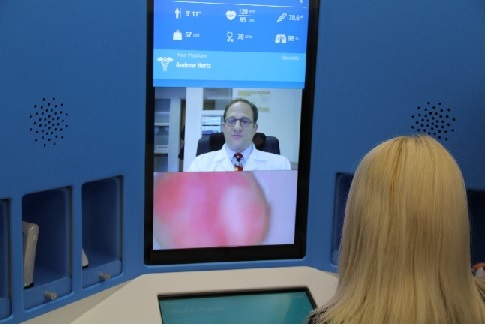
According to IDC’s Connected Health 2014 Predictions, “Retail Clinics Will Disrupt the U.S. Healthcare System”. Most people think about Retail Clinics as a place for getting flu vaccinations or addressing acute problems such as strep throat or ear infections. Retail Clinics are bringing more services to the community and some are now offering preventive services (i.e. physical exams) and chronic disease monitoring.
Over the past two years, RediClinic has been offering a weight management program called Weigh Forward. Shoppers walk into one of their 30 locations inside grocery stores to sign up for the 10- week program. During the initial visit, the clinician does lab work to establish a base line to monitor progress in key health measures. Throughout the program, the clinician provides guidance and teaches life skills not only to lose weight, but keep it off.
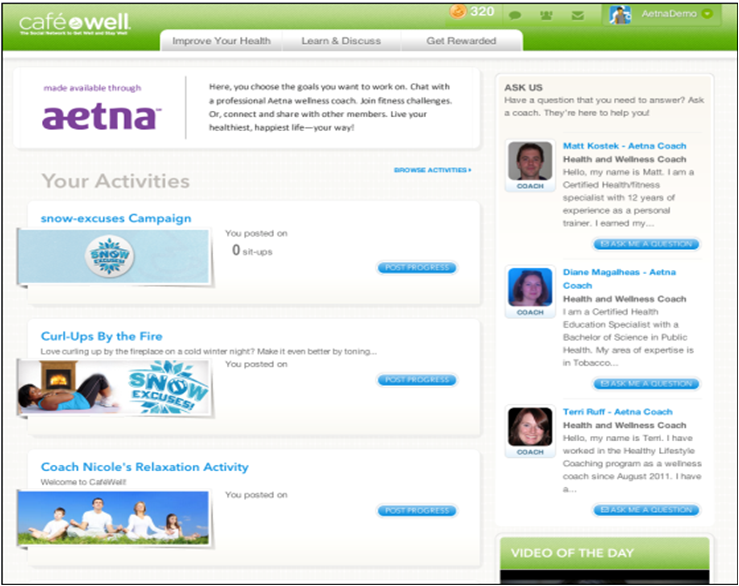
“Our program is a ‘Connected Health’ model. Participants use the MyWeighForward platform to access educational information, track food and physical activity, and receive online coaching and social support between visits to the clinic. During weekly visits to RediClinic, the clinician reviews the participant’s program information (i.e. goals, lab work, tracking information and eCoaching activity) to deliver personalized guidance.”
RediClinic’s Weigh Forward program incorporates four key components which are reinforced both in- person and online through the program’s technology platform – myWeighForward.com:
 RediClinics Patient Portal on MyWeighForward Platform
RediClinics Patient Portal on MyWeighForward Platform
1. Medical. Initial medical assessment with a comprehensive set of lab work, regular biometric monitoring and measurement, and weekly counseling by healthcare professionals.
2. Behavior Modification. Proprietary assessment tool developed at Yale's Prevention Research Center by Dr. David Katz (WeighForward’s Medical Director) to identify and address individual barriers to success and readiness to change, to create a personalized weight loss plan.
3. Diet & Nutrition. Online educational information on food choices, weekly meal plans with 500+ recipes, and access to a diet/nutrition e-coach.
4. Physical Activity. Customized activity plan based on preferences and abilities, access to fitness videos and the capability to collaborate with a fitness e-coach.
Consumer Experience with the Weigh Forward Program
Deborah Hastings signed up for RediClinic's 10- week Weigh Forward program to start shedding 60 pounds. Deborah's daughter is getting married in six months and Deborah wants to get around without pain in her knees and to fit into a new dress for this special event.
During her first appointment, she meets with a clinician for a comprehensive evaluation to discuss her health and weight loss goals and determine her overall health status and readiness for change. She learns that her cholesterol and blood pressure are both high and that she is at risk for Metabolic Syndrome.
She uses the MyWeighForward.com portal to follow a meal plan suggested by the clinician and dietician eCoach, view exercise videos, and to track both her food and physical activity.
 Patient prepares for visit with clinician at RediClinic
Patient prepares for visit with clinician at RediClinic
Deborah is preparing for week #5 visit which is teaching her that it “takes a village” to help her achieve her goals, and she needs support from family, friends and office co-workers. She inputs her Visit objective, completes her checklist of specific tasks and selects a "Barriers to Bust", how to deal with family when they are sabotaging her diet. This barrier is posted on her Visit Plan which she will review with the clinician during her RediClinic visit. While Deborah finishes her homework, her clinician reaches out to the eCoach that Deborah has been working with to discuss nutrition concerns. Within the private clinical portal on the Weigh Forward platform, they discuss strategies for Deborah. During the upcoming visit, Deborah will work with the clinician on the barrier she has selected and will consider suggestions from her eCoach.
Deborah has taken advantage of the social community capabilities on the Weigh Forward platform. She created a profile with demographic information and indicated how much program information to share with other participants. Deborah has decided to share the “Busting the Barrier” badges that she has earned each week. Deborah searched to find others like her and has connected with over a dozen new friends. She has also found an online group with her same barriers and is looking to gain some new real life strategies to address them.
During her week #9 visit, her clinician will take a blood sample to compare key biometric markers to those measured at the beginning of the program. She will be able to view these measures and see her progress in reducing her cholesterol and Metabolic risk in her MyWeighForward program account .
With several months before her daughter’s big event, Deborah is motivated to extend the program. She is planning on paying for the "Boost Maintenance Program with ongoing access to MyWeighForward with e-coaching as needed, monthly clinician visits and weekly in-clinic visits for "body composition analysis/biometrics".
Connected Health Program Engagement & Results
Although the Weigh Forward Program was launched in 2011, it wasn’t until RediClinic moved to the new MyWeighForward Platform powered by Wellness Layers in October 2013 that they were able to offer enhanced functionality and support for patients and clinicians including:
- Personalized Consumer Experience & Outcome: Participants create their own mini- electronic health record which collects program information, preferences, visit planning, tracking data, social engagement and progress through health measures. Program participants have the convenience of seeing different clinicians within the same clinic based on appointment availability or in a different location since all RediClinic clinicians have access to the participant’s program information to deliver a consistently high quality and personalized experience.
- Social Engagement: WeighForward participants use the platform 24x7 for ongoing emotional and educational support through their weight loss journey.
- Clinician Support and Collaboration: Clinicians have their own portal, giving them access to information to support and consistently deliver the program and to privately and securely collaborate on care.
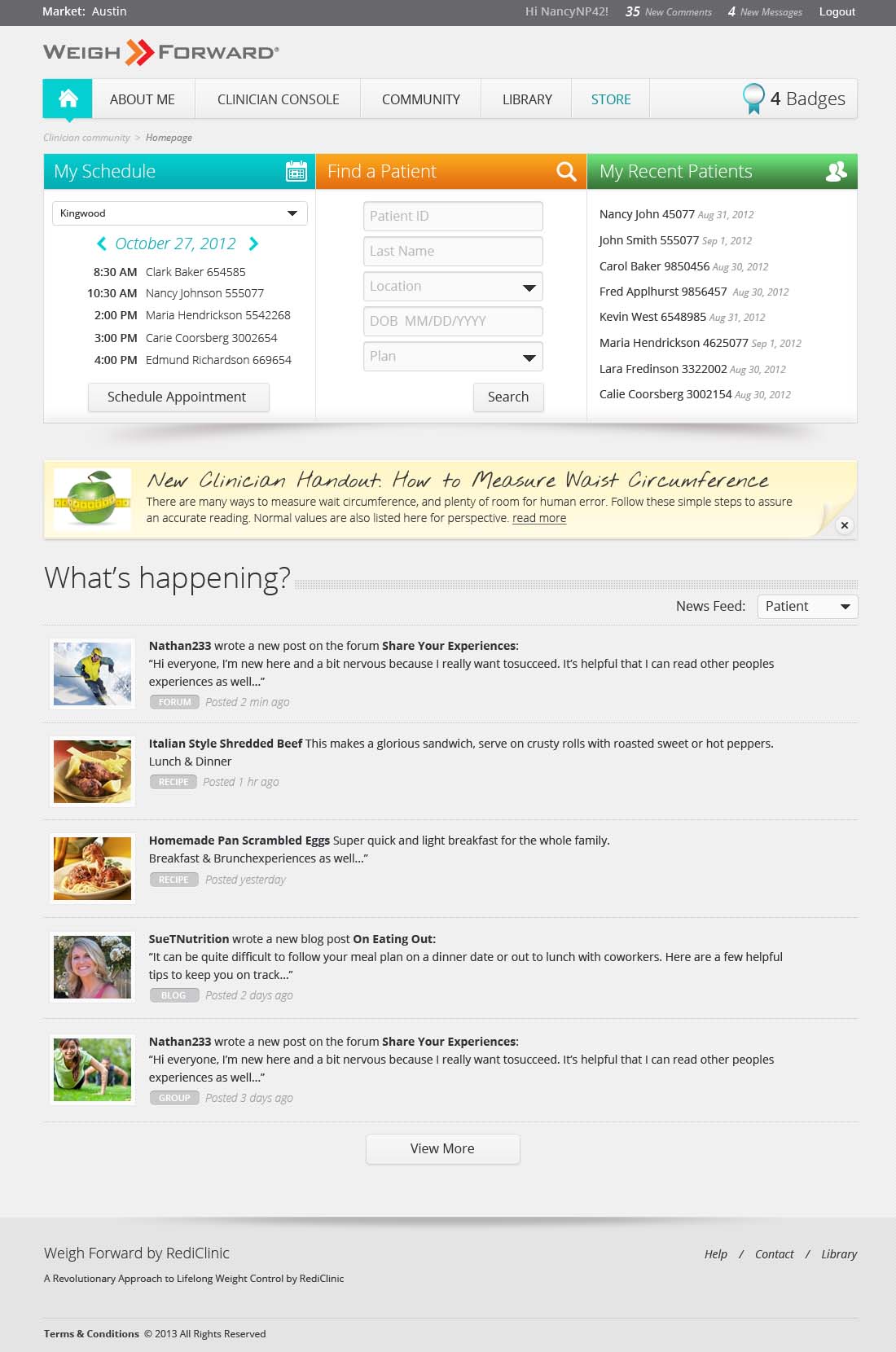 RediClinic's Clinician Portal on MyWeighForward Platform
RediClinic's Clinician Portal on MyWeighForward Platform
- Care Continuum: Participants can access a Program Summary with their program health measures to send to their own doctors. “If the patient has secure messaging with their physician, they can share this information to include in their EMR”, adds Barrera.
“Our results have been very positive. On average, our patients are losing 1- 2 lbs per week which is considered to be a healthy rate of weight loss, and are significantly improving their cardio-metabolic risk factors. In many cases our patients have moved from pre-hypertensive and hypertensive to normal and pre-diabetic to normal”, exclaims Barrera.
Comments from Program Participants
What I liked about the online part of the program was that it gave me homework to do to keep me accountable and focused.
I had been the 'queen of couch potatoes.' The best things about the program were the accountability each week, recipes and shopping list, and incredible support from the staff
Dr. David Katz's lesson on Trial by Aisle taught me to check ingredients lists for hidden sugars and salts, and to pick the shorter lists. The best thing about the program was it provided me with information to change my unhealthy lifestyle into a healthy lifestyle.
Future plans: New Business Model, New Technology Platform Capabilities
Today, most program participants walk into to RediClinic. However, RediClinic is now licensing the Weigh Forward program to other healthcare providers. “We’ve had significant interest and many pilot commitments from large healthcare systems and physician groups, as well as companies that operate retail, urgent care and worksite clinics. Everyone is looking for a turn-key weight and lifestyle management solution for their patients because obesity is so pervasive and expensive. Weigh Forward is one of the few comprehensive programs that is designed to be delivered by clinicians with no previous background in weight management,” Barrera adds.
Regardless of where the consumer is seen, in the clinic or in their PCP’s office, RediClinic is extending the capabilities of the WeighForward technology platform. “We are continuing to enhance the social networking capabilities of the platform, will introduce a mobile version later this year, and are beginning to develop modified versions of Weigh Forward that address chronic diseases, since the platform we’ve built is flexible and extensible”, concludes Barrera.
 educating consumers about health and wellness,
educating consumers about health and wellness,  family ehealth engagement,
family ehealth engagement,  mobile health application,
mobile health application,  online health and wellness coaching,
online health and wellness coaching,  patient ehealth engagement in
patient ehealth engagement in  Behavior Change Health & Wellness,
Behavior Change Health & Wellness,  Connected Health,
Connected Health,  Data Driven Health Engagement,
Data Driven Health Engagement,  Decision Support eHealth,
Decision Support eHealth,  Mobile Engagement Health & Wellness,
Mobile Engagement Health & Wellness,  Patient Engagement,
Patient Engagement,  shared decision making ehealth
shared decision making ehealth